Endoscopic ultrasound-guided injection of coils for the treatment of refractory post-ERCP bleeding
Edson Guzmán-Calderón
, Francisco Ruiz
, Juan Antonio Casellas
, Juan Martinez-Sempere
, Lucía Medina-Prado
, Jose R. Aparicio
超声内镜引导下注入弹簧圈治疗难治性ERCP术后出血
An 82-year-old woman was referred for endoscopic retrograde cholangiopancreatography (ERCP) for choledocholithiasis. After cannulation of the pancreatic duct, transpancreatic sphincterotomy and placement of a 5-fr stent in the pancreas were performed. A fully covered self-expandable metal stent was placed because of persistent post-biliary sphincterotomy bleeding.
一名82岁老年女性患者,因为胆总管结石行ERCP术。胰管插管成功后,做了经胰管的括约肌切开术,并且在胰管内放置了一个5Fr的胰管支架。因为乳头切开后持续出血,还放置了自膨式全覆膜金属支架。
The next day, the patient showed melena, hematemesis, and decreased hemoglobin levels. A gastroscopy was performed and active oozing bleeding from the papilla was evident. Injection therapy with epinephrine and hemoclips was performed. A few hours later, a new episode of hematochezia occurred. Repeat endoscopy showed persistent active bleeding from the papilla ([
Fig. 1]). Hemostatic powder (Hemospray; Cook Medical, Winston Salem, North Carolina, USA) was used ([
Fig. 2]), but the bleeding persisted 24 hours later.
第二天,患者出现黑便、呕血和血红蛋白下降。胃镜检查发现乳头处很明显的活动性出血。于是注射了肾上腺素,并打了止血夹。几小时后,患者又出现黑便。再次行内镜检查发现乳头处仍有持续活动性出血【图1】,应用止血粉(止血喷剂;COOK医疗;Winston Salem,北卡罗来纳州,美国)【图2】,但是之后的24小时仍有持续出血。

图1

图2
Endoscopic ultrasound (EUS) was performed. A curvilinear array echoendoscope (GF-UCT180; Olympus, Tokyo, Japan) that allowed color Doppler imaging was advanced to the second portion of the duodenum to visualize the peripapillary vascular anatomy. An arterial vessel was identified in the duodenal wall at the level of the papilla. EUS-guided embolization was performed with a 0.018” coil (Tornado; Cook Medical, Inc., Bloomington, Indiana, USA) through a 22-gauge needle. Color Doppler imaging confirmed the absence of blood flow after therapy ([
Video 1]). Duodenoscopy was performed immediately after embolization, and the absence of bleeding was confirmed ([
Fig. 3]).
最后做了超声内镜。应用纵轴超声内镜(GF-UCT180; 奥利巴斯, 东京, 日本 )彩色多普勒成像在十二指肠第二段显示乳头周围血管的解剖。在乳头水平的十二指肠壁发现一根动脉血管。超声内镜引导下通过22G穿刺针释放0.018”弹簧圈(Tornado; Cook Medical, Inc., Bloomington, 印第安纳州, 美国)进行栓塞治疗【视频1】。彩色多普勒成像显示栓塞治疗后血流消失。栓塞治疗后立即行十二指肠镜检查确认出血停止【图3】。
|
Video 1Endoscopic ultrasound identified an arterial vessel in the duodenal wall at the level of the papilla. Endoscopic ultrasound-guided embolization was performed with a 0.018” coil through a 22-gauge needle. The absence of blood flow in the blood vessel after therapy was confirmed by color Doppler imaging.
|
|
视频1超声内镜发现十二指肠壁乳头水平处可见动脉血管。超声内镜引导下通过22G穿刺针释放0.018”弹簧圈行栓塞治疗。彩色多普勒成像显示栓塞治疗后血流消失。
|
|
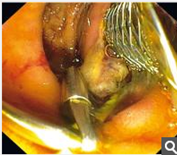
Fig. 3Duodenoscopy was performed immediately after embolization, and the absence of bleeding was confirmed.
图3 栓塞术后行十二指肠镜检查,确认出血停止。
|
The efficacy of EUS-guided treatments of nonvariceal upper gastrointestinal bleeding has been reported only in the form of small case series and case reports [
1]. Fockens et al. [
2] first reported on the usefulness of EUS in the diagnosis and treatment of small abnormal vessels in patients with Dieulafoy’s lesions. Currently, series have been described with success rates of 88 % – 100 % in the treatment of gastrointestinal stromal tumors, Dieulafoy lesions, duodenal ulcers, pancreatic pseudoaneurysms, ulcers related to esophageal cancer, and after Roux-in-Y gastric bypass [
3] [
4] [
5]. EUS-guided injection of coils for the treatment of refractory post-ERCP bleeding has not been reported in the literature.
非静脉曲张的上消化道出血的患者中,应用超声内镜引导下止血只出现在系列病例报道中的个案报道中。Fockens 等第一次报道了超声内镜成功用于溃疡部位小的变异血管的诊断和治疗。
目前,系列报道关于胃肠间质瘤、杜氏病、十二指肠溃疡、胰腺假性动脉瘤、食管癌相关溃疡、Rouen-Y术后出血的治疗有效率为88%-100%。超声内镜引导下弹簧圈治疗ERCP术后难治性出血的报道还很少。
In conclusion, EUS-guided injection of coils is a safe and effective alternative for the treatment of refractory post-ERCP bleeding if other conventional techniques have failed.
总之,对于ERCP术后的难治性出血,在传统止血方法都无效时,超声内镜引导下弹簧圈栓塞治疗是一种安全有效的替代治疗方法。




